First case:
1) What is the reason for this patient's ascites?
Ans: excessive chronic alcohol use can cause chronic liver disease, alcholic fatty liver, alcoholic hepatitis, alcoholic cirrhosis..
In absence of inflammation Or necrosis alcohol use can produce Fibrosis..
The clinical manifestations of cirrhosis include ascites, pedal edema, pain, fever, nausea, development of jaundice( scleral icterus) , upper gi hemorrhage..
In cirrhosis increase in portal hypertension causes sphlancnic vasodilation results in increase portal venous flow... Both these cause increased production of splanchnic lymph.. These hemodynamic changes result in sodium retention by causing activation of RAAS pathway with increase in aldosterone..
Sodium retention causes fluid accumulation and expansion of ecf results in edema and ascites..
2) Why did the patient develop bipedal lymphedema? What was the reason for the recurrent blebs and ulcerations and cellulitis in his lower limbs?
Ans: Bilateral pedal oedema which is of pitting type is due to decrease in the albumin level trends due to course of the disease and long standing cirrhosis causing decrease in the production of proteins causing decrease in the oncotic pressure leading to accumulation of fluid.
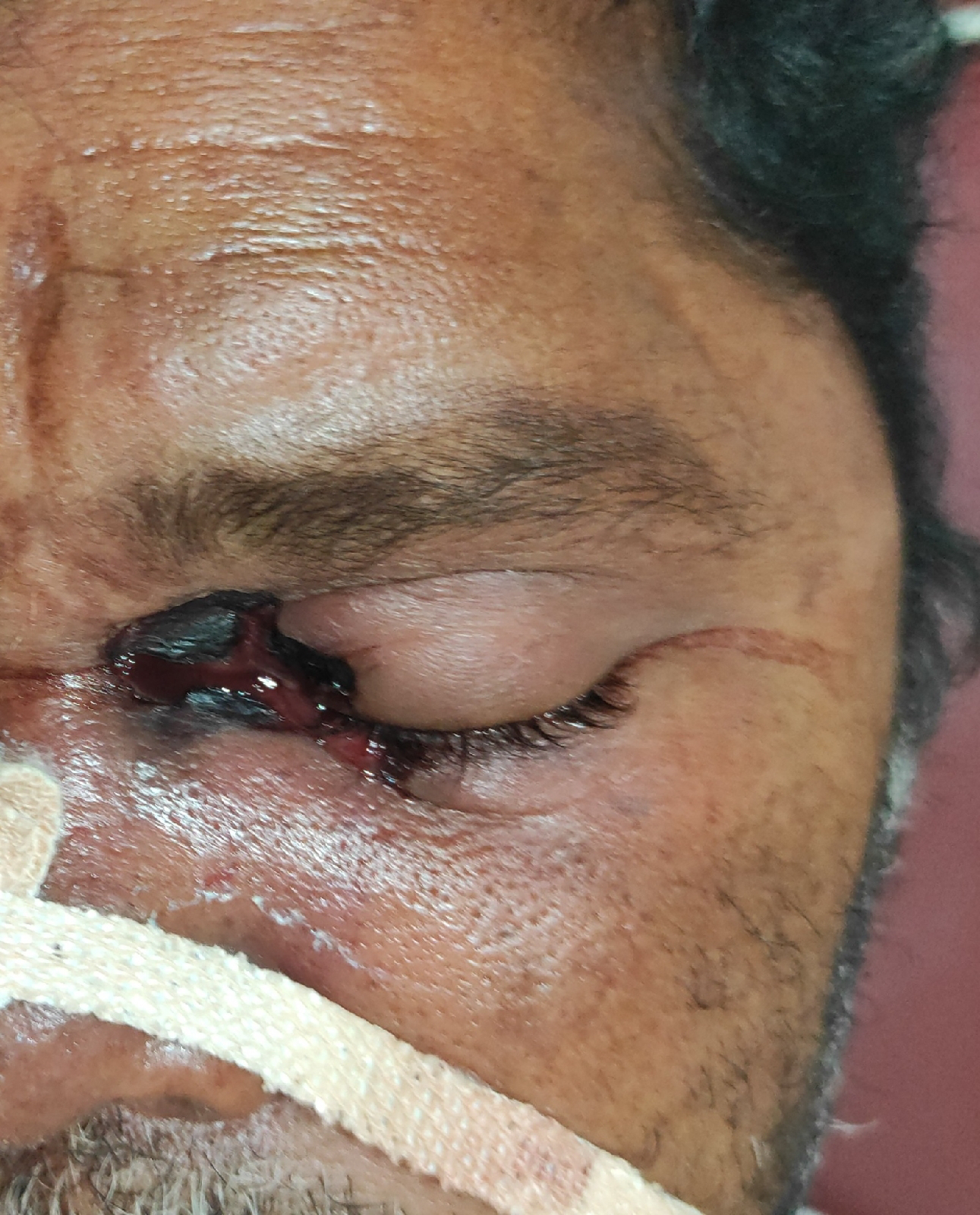
as per the given clinical data due to chronic liver disease there was increasing trend of INR which was as high as 4.7 causing bleeding manifestations ( bleeding gums, hematoma formation )
ulcerations are due his limited self practising manoeuvres done in inappropriate conditions such as
improper dressing of the wound, not maintaining aseptic conditions , indescriminate use of steroids (self medication) causing ? immune suppression leading to secondary infections hence cellulitis and non healing of wound
Lymphedema tarda is a congenital disease characterized by underdevelopment of lymphatic pathways. It manifests as accumulation of lymph in the interstitial spaces of the skin. Wound healing is significantly impaired. Ulcerations which occur during the course of the disease heal slowly or not at all. The cause of this impairment is the continued lymphatic drainage as well as a regional oxygen deficiency in the diseased tissue.
3) What was the reason for his asterixis and constructional apraxia and what was done by the treating team to address that?
Ans: hepatic encephalopathy
the treating team gave
lactulose and rifaximin
underlying mechanism of Giving lactulose
The human small intestinal mucosa does not have the enzymes to split lactulose, and hence lactulose reaches the large bowel unchanged.
basically three mechanisms have been described on usage of lactulose
1.First, the colonic metabolism of sugars causes a laxative effect via an increase in intraluminal gas formation and osmolality which leads to a reduction in transit time and intraluminal pH. This laxative effect is also beneficial for constipation.
2. lactulose promotes increased uptake of ammonia by colonic bacteria which utilize the trapped colonic ammonia as a nitrogen source for protein synthesis. The reduction of intestinal pH facilitates this process, which favors the conversion of ammonia (NH3) produced by the gut bacteria, to ammonium (NH4+), an ionized form of the molecule, unable to cross biological membranes.
3. lactulose also causes a reduction in intestinal production of ammonia. The acidic pH destroys urease-producing bacteria involved in the production of ammonia. The unabsorbed disaccharide also inhibits intestinal glutaminase activity, which blocks the intestinal uptake of glutamine, and its metabolism to ammonia.
4) What was the efficacy of each treatment intervention used for this patient? Identify the over and under diagnosis and over and under treatment issues in the management of this patient.
Ans
Second case :
1) Why were his antitubercular therapy stopped soon after his current admission? Was he symptomatic for ATT induced hepatitis? Was the method planned for restarting antitubercular therapy after a gap of few days appropriate? What evidence is this approach supported by?
Ans:: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5366108/
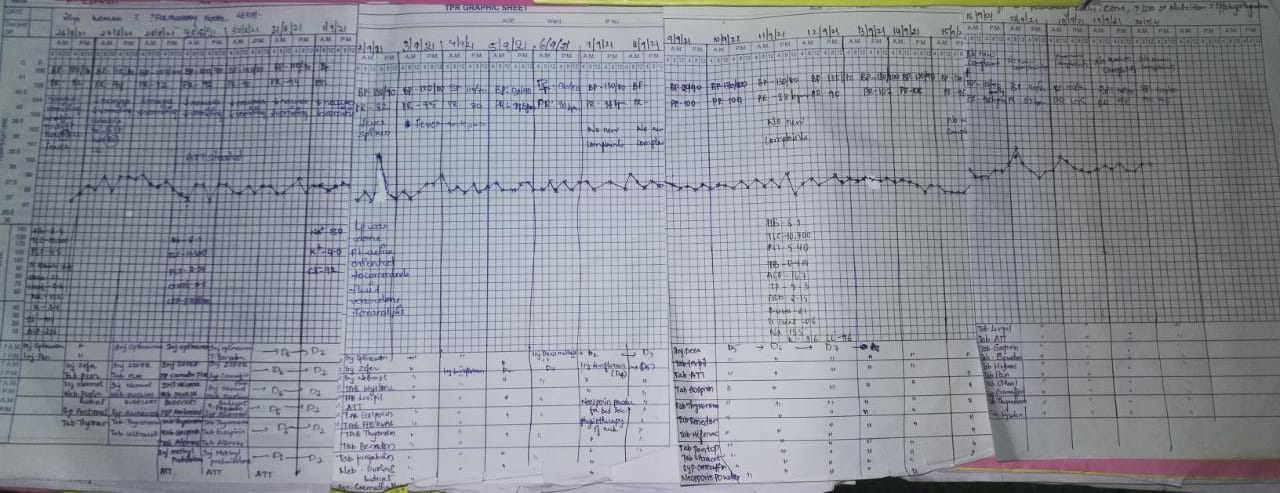
His att was stopped due to altered bilirubin metabolism and increased liver enzymes .. He was sympotomatic for ATT induced hepatitis include yellow skin and eyes (jaundice), nausea, abdominal pain, fatigue and fever which spikes at night
Generalized weakness
Sputum was found positive.
Increased Neutrophil count points to an Active Pulmonary tuberculosis.
Thromocytopenia
Hazy opacities seen on Chest X ray.
CT shows fibrocavitary lesion in right lung.
Patient looks emaciated and has anemia which signify the severity of tuberculosis.
https://clinicaltrials.gov/ct2/show/study/NCT01395654
This clinical trial suggests that It could also be hazardous Reintroducing after att induced hepatitis
2) What were the investigational findings confirming the diagnosis of pulmonary TB in this man?
Ans:: he started having abdominal tightness(after taking spicy foods ),pedal edema - pitting type (on and off) shortness of breath, all symptoms from 1 month for which he was referred to govt hospital where he was diagnosed as sputum positive TB and started ATT
3) What was the cause of his ascites?
Ans: High saag and low ascitic protein Suggestive of cirrhosis is casue for ascites
- LATE BUDD-CHIARI SYNDROME
- HYPOALBUMINEMIA
4) What are the efficacy of each intervention mentioned in his treatment plan and identify the over and under diagnosis as well as over and under treatment issues in it.
Third case ::
1) What will be your further approach toward managing this patient of nephrotic syndrome? How will you establish the cause for his nephrotic syndrome?
Ans:By renal biopsy.....subjected to light , immunofloroscence and electron microscopy... If it is diabetic nephropathy, there is capillary basement membrane thickening with Diffuse glomerulosclerosis as most common finding.. Nodular or intercapillary glomerulosclerosis ( kimmelstein Wilson disease) is the most specific finding... If it is membranous nephropathy there is immune complex deposition giving the appearance of Spike and dome on electron microscopy.. If it is FSGS.. There is focal segmental sclerotic areas because of deposition of IgM and C3 ...but hall mark of FSGS is Visceral epithelial cell damage with diffuse effacement of foot process of viscera epithelial cells on E/M. In fibrillary immunotactoid glomerulopathy fibrillar or microtubular deposits of oligoclonal or oligotypic immunoglobulins and complements appear in the mesangium and along the glomerular capillary wall... In Light chain deposit disease.. The light chain deposits are not fibrillar and don't stain with Congo red, but easily detected with anti light chain antibody using immunofluorescence or granular deposits on electron microscopy.
.Initial management should focus on investigating the cause,
Primary ( idiopathic )
Secondary glomerular pathology
Primary causes include
FSGS
membranous glomerular nephropathy
minimal change
MPGN
Secondary causes of nephrotic syndrome
Infections
HIV
Hepatitis B and C
Mycoplasma
Syphilis
Malaria
Schistosomiasis
Filariasis
Toxoplasmosis
Congenital causes
Alport’s syndrome
Congenital nephrotic syndrome of the Finnish type
Pierson’s syndrome
Nail-patella syndrome
Denys-Drash syndromanaging the symptoms of the disease such as protein , pedal edema
Managing the symptoms of the disease such as protein loss, pedal oedema,
and hyper coagulable state which still did not manifested in this patient or need not be in many
cases.
2) What are the pros and cons of getting a renal biopsy for him? Will it really meet his actual requirements that can put him on the road to recovery?
Ans::
PROS of renal biopsy :
1)Gives a specific diagnosis, reflect the disease activity, provide information to allow decisions and planned treatment..
2)It remains a valuable clinical tool and of particular benefit when other investigations fail to diagnose...
CONS:
1) Dull ache pain around the needle entry site...
2)Sometimes perirenal haematoma forms leading to severe loin pain...
3)The mean decrease in Hb after biopsy is approximately 1g/dl...
4)Visible hematuria in 3.5% ,Need for blood transfusion in 0.9% and need for intervention to control bleeding in 0.7% and Death in 0.02 %....
5)Rare complications include infection, damage to blood vessels or other organs or urine leak... Sometimes development of arteriovenous fistula.